Science is ever changing, thus, so is what we do. If we only stick to what we know now, three to five years down the road.. you might lose your credibility and clientele. We should always strive for excellence and professional advancement. One way to brush up your knowledge and skills is attend seminars and courses of high quality (speakers and organization). I have short listed seminars which I think will help your clinical practice.
A true professional empties his cup to learn and fill his cup with new ideas. He continually seeks for ways to be more efficient and skilled at what he does. As healthcare and medical professionals, it is our duty to give the best quality service to our patients/clients. And, it is only through continuing education that we can be at par and upgrade our clinical practice.
Science is ever changing, thus, so is what we do. If we only stick to what we know now, three to five years down the road.. you might lose your credibility and clientele. We should always strive for excellence and professional advancement. One way to brush up your knowledge and skills is attend seminars and courses of high quality (speakers and organization). I have short listed seminars which I think will help your clinical practice.
0 Comments
Dynamic Concepts Webinar Series: Session 5 American College of Occupational and Environmental Medicine Improving the care and well being of workers through science and the sharing of knowledge presents EVIDENCE BASED TREATMENT FOR |
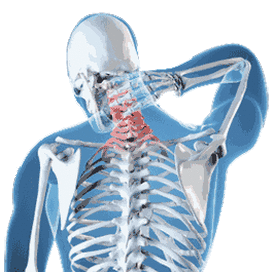
| Learn more about the different cervical and thoracic conditions. The recorded webinar presented last December 6, 2010 talks about signs and symptoms of each disorder for a more accurate diagnosis. It also focuses on evidence based evaluation, assessment and treatment of common cervical and thoracic spinal disorders. *Any CME/MOC credit for this activity mentioned within the presentation has expired and is no longer valid. |
WATCH NOW BY CLICKING ON THE IMAGE >>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>>
CLICK.LEARN.MOVE.
Speaker:
Jeffrey S. Harris, MD, MPH, FACOEM
Senior Physician, The Permanente Medical Group; President, J. Harris Associates, Inc.; Clinical Associate Professor, University of California at San Francisco, University of Utah and Medical College of Wisconsin
Senior Physician, The Permanente Medical Group; President, J. Harris Associates, Inc.; Clinical Associate Professor, University of California at San Francisco, University of Utah and Medical College of Wisconsin
Activities/Associations:
Board of Directors, Finance Committee, Policies and Procedures Committee, ACOEM; President and member of the Board of Directors, Collaborative for Excellence in Occupational Medicine (CEOM); Methodology Committee and Evidence-Based Practice Committee, ACOEM; Consultant, Evidence-Based Medicine Task Force, ACOEM; Associate Chair, Scientific Affairs Committee; Editor, ACOEM Occupational Medicine Practice Guidelines, 1st Edition and Associate Editor, 2nd Edition; past chair, Practice Guidelines Committee, ACOEM, 1994-98; Guideline Quality Review Committee, The Permanente 6 Federation/Care Management Institute; Reviewer, the Cochrane Collaboration, Musculoskeletal and Low Back Groups and Occupational Medicine Field; and American College of Physicians/American Pain Society Low Back Guideline. - See more at: ACOEM website
Board of Directors, Finance Committee, Policies and Procedures Committee, ACOEM; President and member of the Board of Directors, Collaborative for Excellence in Occupational Medicine (CEOM); Methodology Committee and Evidence-Based Practice Committee, ACOEM; Consultant, Evidence-Based Medicine Task Force, ACOEM; Associate Chair, Scientific Affairs Committee; Editor, ACOEM Occupational Medicine Practice Guidelines, 1st Edition and Associate Editor, 2nd Edition; past chair, Practice Guidelines Committee, ACOEM, 1994-98; Guideline Quality Review Committee, The Permanente 6 Federation/Care Management Institute; Reviewer, the Cochrane Collaboration, Musculoskeletal and Low Back Groups and Occupational Medicine Field; and American College of Physicians/American Pain Society Low Back Guideline. - See more at: ACOEM website
Bringing Out The Evidence of Lack of Evidence Based Practice
How many times have you treated a certain case with the same management over and over again with different patients? Have you ever given the same home exercise program handouts to patients of similar diagnosis? Was there a time you did special tests and measures but it did not yield a positive result to the condition? Are you guilty of all of these? I know I was.
This is just proof that we are not as committed to incorporate evidence based practice in our profession. We know well that every patient no matter how similar the case may be will have a different response to an assessment or treatment. We also know pretty well that patient’s compliance to physical therapy sucks as hell. But because handing out HEPs (as Ryan Kelps points out) is easier, we just go with it. Same goes for the monotonous treatment protocols we provide to patients.
The problem does not lie with the patients being lazy but US being lazy. We do not give them the support they need. When, as a matter of fact, there many materials out there to work with; that will make them more compliant. This is where evidence based practice comes into play.
This is just proof that we are not as committed to incorporate evidence based practice in our profession. We know well that every patient no matter how similar the case may be will have a different response to an assessment or treatment. We also know pretty well that patient’s compliance to physical therapy sucks as hell. But because handing out HEPs (as Ryan Kelps points out) is easier, we just go with it. Same goes for the monotonous treatment protocols we provide to patients.
The problem does not lie with the patients being lazy but US being lazy. We do not give them the support they need. When, as a matter of fact, there many materials out there to work with; that will make them more compliant. This is where evidence based practice comes into play.
Dynamic Concept Series 4: Positional Release of The Spine with Dr. Leon Chaitow
| As presented by Hands On Seminars: Manual Therapy Training Education 'The leading continuing education organization with a purpose to provide the best quality Manual Therapy seminars at an affordable cost.' |
Positional Release Technique was based on strain - counterstrain (by Lawrence Jones, DO) and was developed by George Roth, Kerry D’Ambrogio and other pioneers of musculoskeletal therapy. It is a non-traumatic manual therapy technique to treat neuromuscular and musculoskeletal disorders or basically those with somatic dysfunction. Assessment and treatment utilizes tender points and the patient's position of comfort. It causes a positive change in muscle activity , sympathetic nervous system and circulation by applying forces AWAY from resistance.
The body is a pretty amazing work of art. It always has a way to seemingly work in an almost perfect condition even when in pain and distress. That's why it takes a good physio to really pinpoint where the pain truly comes from, why it happened and how. Finding out the REAL CAUSE of the problem makes everybody's job easier (PT, patient, family...).
Usually, we (especially osteopaths) call most of the problems as somatic dysfunctions. What is it exactly? A somatic dysfunction is an "impaired or altered function of related components of the somatic (body framework) system: skeletal, arthrodial, and myofascial structures, and related vascular, lymphatic, and neural elements.” (Glossary Review Committee, for the Educational Council on Osteopathic Principles and the American Association of Colleges of Osteopathic Medicine.Glossary of Osteopathic Terminology. April 2002) Thank you God for giving us physios clues to identify dysfunctions in the body. And there are plenty! The question is how do we know which one is the main perpetrator. Which are the ones we should prioritize and focus on?
If you are having a hard time understanding pain, how the body reacts and adapts to it...
If you want to enhance your clinical reasoning skills...
If you get confused in global and local pattern relationships...
If you want a more efficient and effective way to assess patients...
If you find it difficult to treat chronic pain patients (low back pain, MPS, fibromyalgia, CRPS..)...
If you want to be a better professional...
Usually, we (especially osteopaths) call most of the problems as somatic dysfunctions. What is it exactly? A somatic dysfunction is an "impaired or altered function of related components of the somatic (body framework) system: skeletal, arthrodial, and myofascial structures, and related vascular, lymphatic, and neural elements.” (Glossary Review Committee, for the Educational Council on Osteopathic Principles and the American Association of Colleges of Osteopathic Medicine.Glossary of Osteopathic Terminology. April 2002) Thank you God for giving us physios clues to identify dysfunctions in the body. And there are plenty! The question is how do we know which one is the main perpetrator. Which are the ones we should prioritize and focus on?
If you are having a hard time understanding pain, how the body reacts and adapts to it...
If you want to enhance your clinical reasoning skills...
If you get confused in global and local pattern relationships...
If you want a more efficient and effective way to assess patients...
If you find it difficult to treat chronic pain patients (low back pain, MPS, fibromyalgia, CRPS..)...
If you want to be a better professional...
If you missed out on last month's webinar about chronic pain and how it affects movement, here is an outline of what was discussed. I transcribed the discussion for those who don't have time to listen and watch the recorded webinar. But if you want a more detailed explanation, you can always watch it HERE.
HOW TO USE MOVEMENT WITH GRADED EXPOSURE TO PAIN
Outline:
I. How to use movement and graded exposure to reduce pain?
II. Changes in the nervous system when pain persists
III. Neuroplasticity and potential for change
IV. Influence movement and activity on pain and ability to perform activity without increases in pain
V. Three strategies to use this information:
A. Frequent movement that do not increase your pain
B. Novel movements
C. Graded exposure or gradual activity
I. How to use movement and graded exposure to reduce pain?
II. Changes in the nervous system when pain persists
III. Neuroplasticity and potential for change
IV. Influence movement and activity on pain and ability to perform activity without increases in pain
V. Three strategies to use this information:
A. Frequent movement that do not increase your pain
B. Novel movements
C. Graded exposure or gradual activity
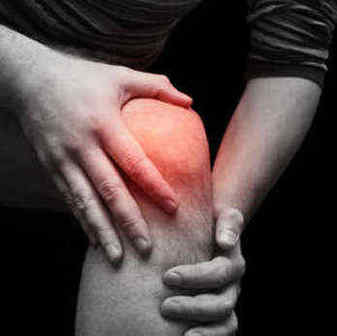
Patellofemoral pain syndrome (PFPS) has been one of the most common knee problems affecting adolescents and active young individuals.1 Up to now; there is no identified single biomechanical factor to its causality. The conventional intervention used to treat PFPS is quadriceps strengthening, specific VMO strengthening, bracing, taping and stretching.3 Little is known whether trunk and hip stabilization exercises may be a better treatment rather than the usual knee exercises.
In the recent October issue of The International Journal of Sports Physical Therapy, a systematic review about the effectiveness of proximal exercises to PFPS was presented. The main objective of the study was to investigate whether the use of proximal exercises will improve pain and function for patients with PFPS.
Before delving into the study, let’s get to know PFPS a little bit more…
In the recent October issue of The International Journal of Sports Physical Therapy, a systematic review about the effectiveness of proximal exercises to PFPS was presented. The main objective of the study was to investigate whether the use of proximal exercises will improve pain and function for patients with PFPS.
Before delving into the study, let’s get to know PFPS a little bit more…





 RSS Feed
RSS Feed






